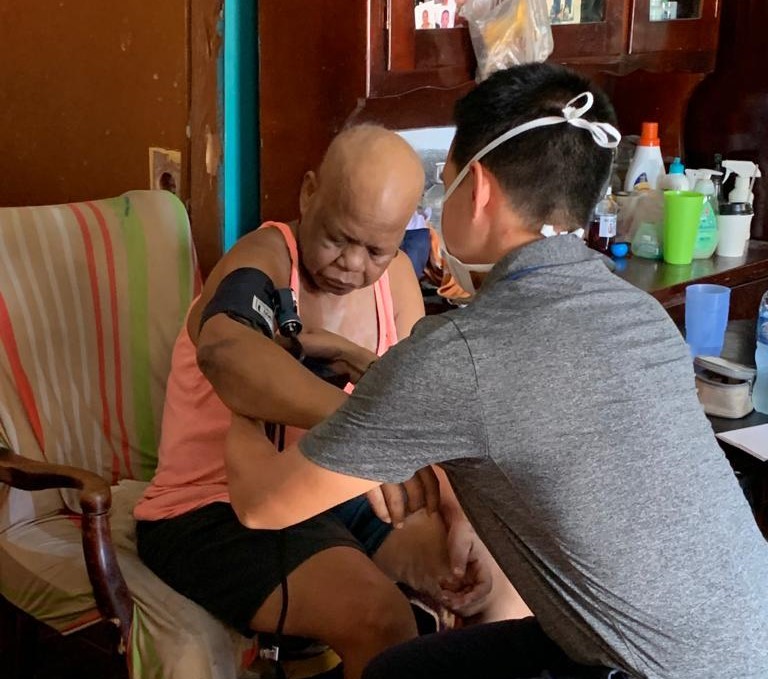
Palliative care is an approach that improves the quality of life of patients and their families facing the problems associated with life-threatening illness through prevention and relief of suffering through: early identification impeccable assessment treatment of pain and other physical, psychosocial, and spiritual symptoms.
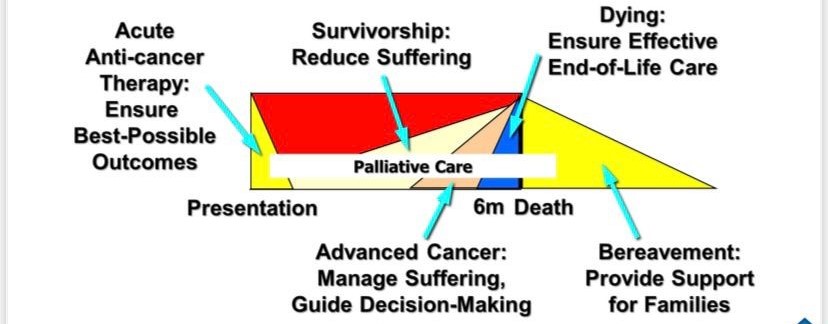
A set of services focused upon relief of suffering and enhancement of quality of life. It is a funding/service delivery model for palliative care It is typically provided during The last phase of an advanced illness Six months Bereavement.
Increasingly, people are choosing hospice care at the end of life. Hospice care focuses on the care, comfort, and quality of life of a person with a serious illness who is approaching the end of life.
At some point, it may not be possible to cure a serious illness, or a patient may choose not to undergo certain treatments. Hospice is designed for this situation. The patient beginning hospice care understands that his or her illness is not responding to medical attempts to cure it or to slow the
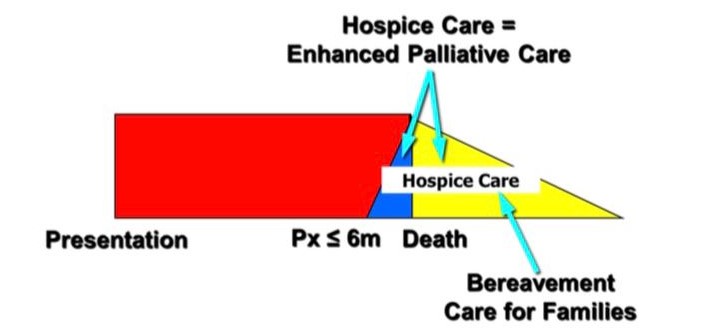
- Appropriate with any serious illness, regardless of stage or ability to cure...
Expert physicals on emotional, spiritual and social symptom management
Navigation of the complex decisions that always come with serious illness
Communication between patients, families, medical professionals and the medical system
Palliative Care focuses more on living than on dying!
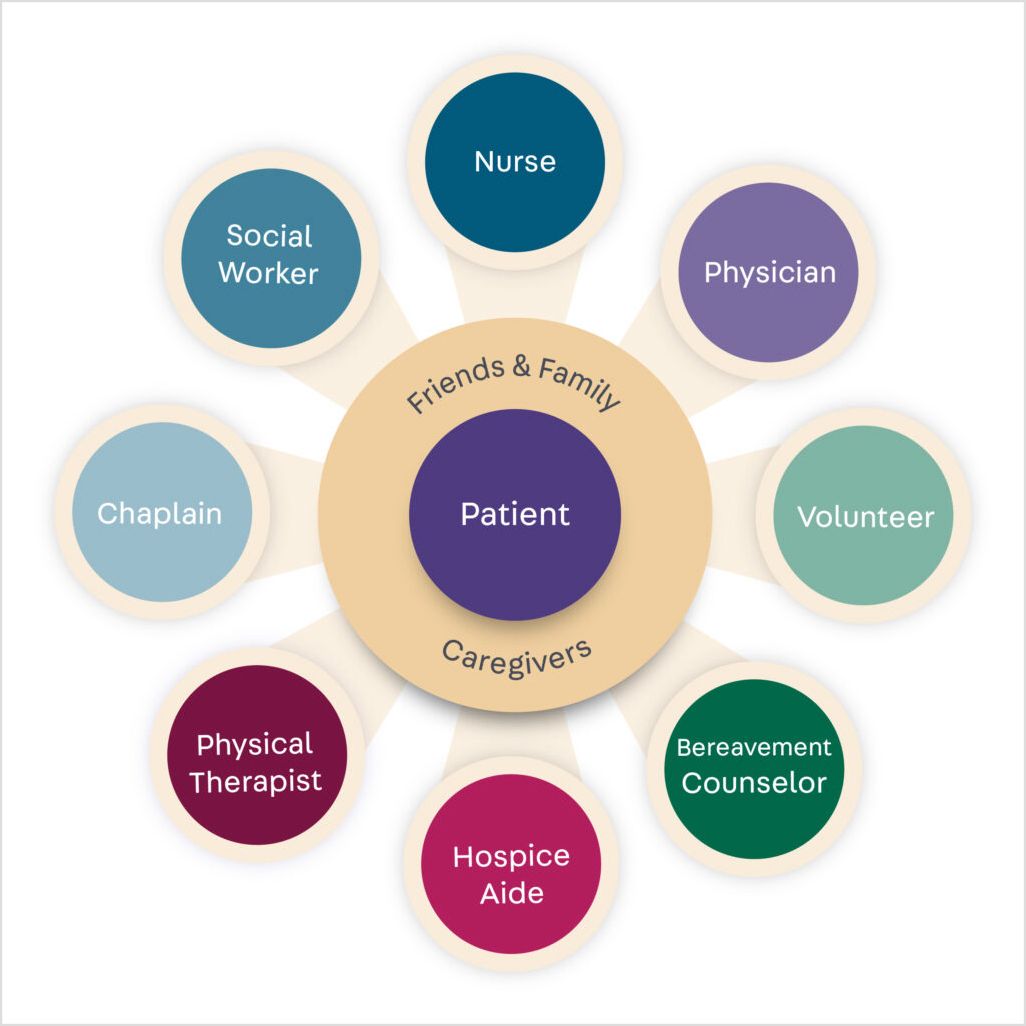
A Transdisciplinary Team Approach service where each professional caregiver is the expert specialist in their own role and becomes a generalist of the other expertise roles in the team. Openness to learn to identify the patient’s urgent needs, address them, and make a referral to the specialist on the team for that aspect is needed.
- The care approach is a “Holistic Approach” to the person experiencing illness and must address the whole person, including the physical, spiritual, social, and emotional dimensions. The spiritual may or may not present religious aspects at this dimension's core. The avoidance of neglecting this dimension results in care that is not palliative care.
- Patients and Family Members are the Unit of Care; they are the center of this organization's care, and the human and material resources are available to them according to their needs.
Palliative care is focused on relief of the pain, stress, and other debilitating symptoms of serious illness. It is not dependent on prognosis and can be delivered at the same time as treatment that is meant to cure. The goal is to relieve suffering and provide the best possible quality of life for patients and their families. Palliative care can be customized to meet the individual needs of the patient.
Palliative care provides support and care for persons in the last phases of an incurable disease so that they may live as fully and as comfortably as possible. This care recognizes that the dying process is a part of the normal process of living and focuses on enhancing the quality of remaining life. Palliative care affirms life and neither hastens nor postpones death. Palliative care seeks to preserve and promote the inherent potential for growth within individuals and families during the last phase of life. Palliative care offers palliative care for all individuals and their families without regard to age, gender, nationality, race, creed, sexual orientation, disability, diagnosis, availability of a primary caregiver, or ability to pay.
Palliative care provides supportive services to individuals at the end of their lives, their family members and significant others, 24 hours a day, seven days a week, in both the home and facility-based care settings. Physical, social, spiritual, and emotional care is provided by a clinically interdisciplinary/transdisciplinary team consisting of patients and their families, professionals, and volunteers during the:
1. Last stages of an illness.
2. Dying process; and
3. Bereavement period.
The National Hospice and Palliative Care Organization (NHPCO) defines palliative care as treatment that enhances comfort and improves the quality of an individual’s life during the last phase of life. No specific therapy is excluded from consideration. The test of palliative care lies in the agreement between the individual, physician(s), primary caregiver, and the hospice team that the expected outcome is relief from distressing symptoms, the easing of pain, and/or the enhancing the quality of life. The decision to intervene with active palliative care is based on an ability to meet stated goals rather than affect the underlying disease. An individual’s needs must continue to be assessed and all treatment options explored and evaluated in the context of the individual’s values and symptoms. The individual’s choices and decisions regarding care are paramount and must be followed at all times.
According to the World Health Organization (WHO), palliative care is defined as the active total care of patients whose disease is not responsive to curative treatment. The term palliative care often is used interchangeably with hospice care, and its goal is to ensure that the patient and family achieve the best possible quality of life (Kim, Wang & Fall, 2005).
The palliative care is provided by a team of professionals that will come to the patient’s place of residence, evaluate, and treat their symptoms to maintain maximum comfort. Professional care is delivered by a staff specialist focused on listening and responding to the patient, the patient’s family, and the patient’s overall healthcare needs. Staff for these services include skilled, chaplain, social worker, nurses, physician, home care aides, and volunteers.
Scope of Services to be provided by the Palliative Care Hospice Association of Belize shall be determined after conducting an “whole person” assessment of the patient and family needs.
Care services provided may include:
- Clinical Services
- Spiritual and Religious Support Services
- Social Work Services
- Nursing Services
- Physician Services
- Volunteer Family Support Services
- Bereavement Services
- other specialties
The interdisciplinary/transdisciplinary care team will coordinate and share information regarding plan of care, provide support for decision-making, develop, and implement care plan, and communicate palliative care initiative to the patient and family and to all involved health professionals. The team will communicate regularly to plan, review, and evaluate the care plan with input from both family and patient.
A unique aspect of the care team is the transdisciplinary team approach nature, breaking away from the medicalize classic medical approach, where the physician is the leading role in the care above all the other specialties. Each role it is the “specialist” on their field in the team and it becomes a “generalist” for the other specialties on the team, as a generalist is able to identify the patient needs and make the referral sooner to the specialist in that domain.
The palliative care transdisciplinary roles can be directed by a social worker, chaplain, and a nurse, not necessary by a physician. Each of these roles are a certified specialty in the palliative care and hospice field equipped with a specific set of skills and training.
Members of an interdisciplinary care team may include the following:
- executive director – Chaplain Frederico Gianelli, S.J.
- clinical director – Dr. Martha Habet / Dr. Ramoncito Yacab
- chaplain – Chaplain Frederico Gianelli, S.J. BCC-PCHAC
- social workers – Intern SW rotating in the service from University of Belize
- practical nurses – Central Health Region and volunteers
- staff nurses – Central Health Region and volunteer
- physician – Central Health Region and volunteer
- bereavement – Chaplain Frederico Gianelli, S.J.
- volunteer services – Volunteer Coordinator Ava Pennil
The values, ethics, and standards of each member of the interdisciplinary team shall guide their decisions and practice in palliative care. Each member of the interdisciplinary team must be prepared for the challenges of ethical dilemmas and values of conflicts and consider questions related to religion, spirituality and the meaning of life. It is recommended that each member of the interdisciplinary team have an understanding of the following ethical principles: Justice: the duty to treat all fairly, distributing the risks and benefits equally Beneficence: the duty to do good, both for individuals and for all Nonmaleficence: the duty to cause no harm, both for individuals and for all Understanding/Tolerance: the duty to understand and to accept other viewpoints, if reason dictates that doing so is warranted Respect for the person: the duty to honor others, their rights, and their responsibilities, as showing respect for others implies that we do not treat them as a mere means to our end Universality: the duty to take actions that hold for everyone, regardless of time, place, or people involved Veracity: the duty to tell the truth Autonomy: the duty to maximize the individual's right to make his or her own decisions Confidentiality: the duty to respect privacy of information and action Equality: the duty to view all people as moral equals Finality: the duty to take action that may override the demands of law, religion, and social customs
The patient, their caregiver/s and family are considered the unit of care. The needs of individual members of unit of care need to be identified and addressed individually.
Quality Palliative Care is provided to the unit of care by health care workers who:
Endeavor to maintain the dignity of the patient, their caregiver/s and family.
Work with the strengths and limitations of the patient and their caregiver/s and family to empower them in managing their own situation.
Act with compassion toward the patient and their caregiver/s and family
Consider equity in the accessibility of services and in the allocation of resources.
Demonstrate respect for the patient, their caregiver/s and family.
Advocate on behalf of the expressed wishes of patients, caregiver/s, families and communities.
Are committed to the pursuit of excellence and the provision of care and support; and
Are accountable to patients, caregiver/s, families and the community
Open and respectful communication with the patient, their caregiver/s and family will facilitate the sharing of relevant information regarding cultural beliefs and/or practices that may be beneficial to holistic well-being. Each member of the interdisciplinary team shall be aware of their own beliefs, values, and feelings and how their personal self may influence their practice.
The cultural background, concerns and needs of the patient and their family are identified and documented in the plan of care. Communication with patient and family is respectful of their cultural preferences regarding disclosure and decision-making. The interdisciplinary team aims to respect and accommodate the range of dietary and ritual practices of patients and their families.
The palliative care program is committed to continuous quality improvement in clinical and management practices. The palliative care program must be committed to the pursuit of excellence and the best quality of care and support for patients and families. Determining quality requires regular and systematic measurement, evaluation, goal setting, and revision of the processes and outcomes of care provided by the program.
Quality care must incorporate attention to:
Patient-centered care, based on goals and preferences of the patient and family
Equity, care that is available to all in need and who could benefit
Efficiency, care designed to meet the actual needs of the patients so that it does not waste resources
The review of clinical, psychosocial and spiritual aspects of care will assess the effectiveness of treatment as documented and lead to change in clinical practices as appropriate. Quality improvement activities are routine, reported and are shown to influence clinical practice. Quality improvement activities for clinical services are interdisciplinary and focused on meeting the identified needs of patients and their families.
The palliative care association of Belize shall have in place a program of education and training that includes:
• On-going continuing professional development for the palliative care team
• A program of awareness on palliative care for fellow professionals
• An education program on palliative care for medical/nursing students
• An education program on palliative care for volunteers
• An awareness program on the availability of palliative care for the public